The American Academy of Pediatrics claims to support the health of all children. Many doctors are appalled by its prescriptions
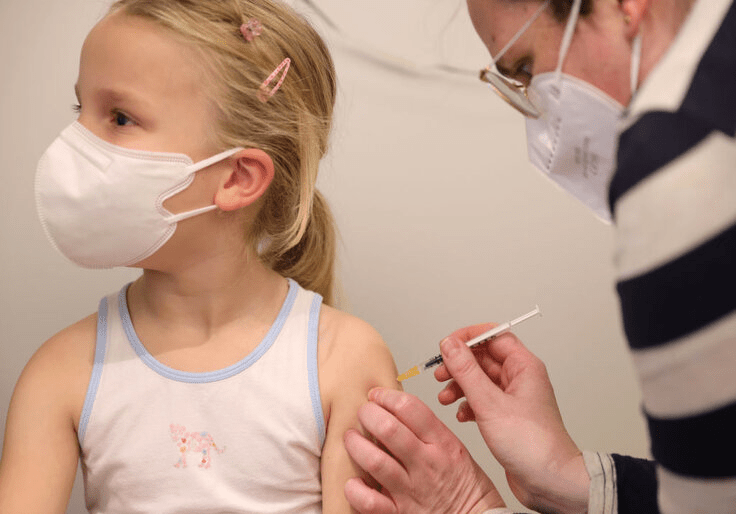
A child in Germany receives a COVID-19 vaccine / Getty Images – The utter foolishness of giving a largely untested and completely unnecessary vaccine to a child wearing the conditioning mask. Children 18 and under have a nearly zero % chance of either getting seriously ill or dying of Covid-19.
Aaron Sibarium • December 7, 2022 5:00 am – for The Washington Free Beacon
The Washington Free Beacon is proud to co-publish this piece with our friends at Common Sense, where it also appears today.
Thousands of pediatricians convened in Anaheim, Calif., in early October for the American Academy of Pediatrics’s (AAP) annual conference. The group, which boasts 67,000 members in the United States and around the world describes itself as “dedicated to the health of all children.”
So some audience members were shocked when Dr. Morissa Ladinsky, an associate professor of pediatrics at the University of Alabama at Birmingham, lauded a transgender teenager for committing suicide.
In an address about “standing up for gender-affirming care,” Ladinsky eulogized Leelah Alcorn, an Ohio 17-year-old who, in Ladinsky’s words, “stepped boldly in front of a tractor trailer, ending her life,” in 2014, after leaving a suicide note that “went viral, literally around the world.”
Ladinsky’s remarks were captured on video by a horrified onlooker, Oregon pediatrician Dr. Julia Mason, who expressed outrage on Twitter that Ladinsky was “glorifying suicide,” an act she described as “unprofessional and dangerous.”
That isn’t just Mason’s opinion. Technically speaking, it is also the official stance of the AAP, whose website for parents, healthychildren.org, explicitly warns that “glorifying suicide” can have a “‘contagious’ effect” and inspire others to take their own lives.
Reached for comment, Ladinsky expressed “regret” about her choice of words and said it was “never my intent” to glorify self-harm.
But how did this esteemed doctor wind up telling a group of physicians that a teen had, as she put it, “boldly ended her life?”
In any large organization, some members are bound to hold fringe views. But Ladinsky, who has devoted her career in part to facilitating the gender transition of teenagers including by challenging state laws that restrict the kinds of treatment physicians can provide to them, is hardly an outlier at the AAP. And the AAP is an organization that matters a great deal.
Founded in 1930 as an offshoot of the American Medical Association, the AAP is first and foremost a standard-setting body. It outlines best practices for the nation’s pediatricians, advises policy-makers on public health issues, and, for many parents, is the premier authority on raising healthy kids.
In recent years, it has also become a participant in America’s culture wars. Judges have deferred to the group’s expertise in high-stakes court cases about children with gender dysphoria, who the AAP says can start socially transitioning at “any” age. During the height of Covid, schools masked toddlers—including toddlers with speech delays—based on the guidance of the AAP. Sports leagues and after-school programs mandated the Covid vaccine after the AAP strongly recommended it, even as concerns mounted about its association with myocarditis, or inflammation of the heart muscle, in young males.
Though the organization’s guidelines are framed as the consensus position of the AAP’s members, only a handful of physicians had a role in shaping them. Instead, insiders say, the AAP is deferring to small, like-minded teams of specialists ensconced in children’s hospitals, research centers, and public health bureaucracies, rather than seeking the insights of pediatricians who see a wide cross-section of America’s children.
They also say a longstanding left-wing bias—over two thirds of pediatricians are registered Democrats—has accelerated, turning the organization into a more overtly political body that now pronounces on issues from climate change to immigration. As rates of gender dysphoria exploded and the Covid-19 pandemic hit, that bias seeped into the organization’s medical policy recommendations, unchecked by discussion or debate.
This story is based on dozens of interviews with pediatricians, academics, and current and former AAP members, including several with leadership positions in the AAP. It shows how a small group of doctors with virtually unaccountable power can exert tremendous influence over public policy, especially when a new crisis—be it moral or virological—gives them an emergency mandate. A mandate affecting the lives of millions of families.
Covid: ‘Political Science Over True Science’
In the last week of June 2020, with no end to the pandemic in sight, the AAP took a strong stance against school closures.
“The importance of in-person learning is well-documented, and there is already evidence of the negative impacts on children because of school closures in the spring of 2020,” the group said in a statement, which listed a litany of maladies—learning loss, food insecurity, isolation, depression, physical and sexual abuse, substance use, suicidal ideation—that could result from prolonged shutdowns. “[A]ll policy considerations for the coming school year should start with a goal of having students physically present in school.”
Then, on July 6, then President Donald Trump tweeted: “SCHOOLS MUST OPEN IN THE FALL!!!”
Over the next week, administration officials from Vice President Mike Pence to Education Secretary Betsy DeVos cited the AAP in the course of pressuring local officials to reopen schools.
It didn’t take long for the AAP to buckle. By July 10, the organization issued a follow-up statement—this one co-authored with the teachers unions—suggesting that in-person schooling would be impossible without “substantial new investments” from the federal government. Most European children, meanwhile, returned to the classroom.
It was a microcosm of the AAP’s handling of the pandemic: From masking toddlers to boosters for 12-year-olds, the group’s guidelines were consistently out of sync with those of the rest of the world, but very much in line with the demands of anti-Trump partisans.
“The AAP cared much more about political science than true science,” one pediatrician said.
When schools began to reopen, at first in red states, the group advised that every child, including toddlers, should remain masked for the duration of the day—despite the fact that the AAP had until then stressed the importance of facial cues for early childhood development—even as most other Western countries opted against masking young kids.
The organization didn’t just recommend masks; it lobbied politicians to require them.
In an August 2021 email obtained by Common Sense and the Washington Free Beacon, the Colorado chapter of the AAP, acting on the policy recommendations adopted by the national organization, urged members to contact the state’s governor expressing support for a mask mandate in Colorado public schools. Three months later, the Iowa chapter submitted an amicus brief challenging a state law that prohibited school mask mandates.
These moves prompted outrage from many rank-and-file pediatricians, several of whom contacted AAP leaders with concerns about the group’s Covid recommendations, emails obtained by Common Sense and the Free Beacon show. Masks “really hinder speech and socialization for the child care/preschool set,” one pediatrician, who requested anonymity, wrote to Lee Beers, the then-president of the AAP, in April 2021, noting that for these reasons the World Health Organization advises against masking children under six.
Beers forwarded the email to Heather Fitzpatrick, a member of the AAP’s Covid-19 response team, who thanked the concerned pediatrician for sharing the perspective but did not follow up on the substance. Other doctors reported similar stonewalling.
As recently as August 2022, the AAP tweeted that “there is no evidence” that masks can harm childhood language development.
But prior to the pandemic, the AAP itself had argued that seeing faces is critical for early childhood development.
According to Developmental and Behavioral Pediatrics, a book published by the AAP in 2018, visually impaired children “are slower to acquire adjectives and verbs” than their sighted peers, and, at younger ages, are less likely to smile because “smiling is learned by seeing others smile”—findings that raise obvious concerns about masks in schools. In the August 2022 tweet, however, the AAP asserted that “visually impaired children develop speech and language at the same rate as their peers.”
Another AAP publication, this one geared toward parents and available at least since 2013, emphasized the link between “face time” and “emotional health”—only for the document to disappear from the AAP’s website during the pandemic. An AAP spokesperson attributed the disappearance to a “web content migration” and said it had “nothing to do with AAP’s mask guidance,” telling Reuters that the document would be republished on a new platform.
It never was: When Common Sense and the Free Beacon asked to be directed to the document’s new home, a spokesperson for the AAP said it “was removed because it was outdated.”
The AAP has also been exceptionally aggressive in its promotion of Covid-19 boosters for children, which have been linked to myocarditis, a potentially dangerous heart condition, especially in young men. The link is strong enough, and the risk of pediatric Covid low enough, that most European countries did not offer healthy adolescents a third shot, let alone a fourth, while a few stopped vaccinating healthy children against Covid entirely.
The AAP didn’t stop at advocating a third dose of the original vaccine, however. In September, it recommended that every child 12 years and older additionally receive the updated, “bivalent” Covid booster— regardless of whether they also had natural immunity from contracting Covid, and despite the fact that healthy children rarely become seriously ill from the virus.
Parents hesitant about the new booster, which was only tested in eight mice, were told they shouldn’t be. The AAP’s booster recommendations do not include an exemption for children with a history of myocarditis, unless the condition was vaccine-related, because, as an article on healthychildren.org, an AAP publication for parents, puts it: “Compared to the potential risks of Covid-19 infection in kids, myocarditis appears to be quite rare.”
What the group doesn’t tell parents is that all of these recommendations were the product of approximately a dozen doctors on an ad hoc “Covid-19 response team,” which operated in such an opaque manner that many AAP members were unaware of its existence.
“I have no idea who made these decisions,” said Eliza Holland, a pediatrician at UVA Children’s hospital. “I wasn’t even aware a Covid committee exists,” another pediatrician said.
There is no record of the Covid-19 response team anywhere on the AAP’s website, and the organization declined to provide a list of its members. Even AAP officials who knew about the committee could only name a handful of people on it, based on sporadic interactions with the group.
One name that kept coming up was Yvonne Maldonado, the former chair of the AAP’s committee on infectious disease and a professor of pediatrics at Stanford Medicine.
While not the head of the response team, Maldonado appears to have been in the driver’s seat on many of its key decisions. She was quoted in AAP press releases about the pandemic and, from August 2021 to June 2022, served as the AAP’s main representative on the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices, which draws up vaccine recommendations for children.
Maldonado, who did not respond to request for comment, also ran clinical trials of Pfizer’s mRNA vaccine at Stanford—a job for which she would have been paid, according to the company’s guidelines on clinical trials.
The AAP said that Maldonado complied with all of its conflict of interest disclosure policies. But her work with Pfizer may help explain why the AAP and CDC—while notionally separate institutions—have issued nearly identical recommendations on the Covid vaccine, parlaying the views of a few academics into a government-wide consensus that has affected millions of children.
“Very few people are behind these sweeping policies,” said Ram Duriseti, an associate professor of emergency medicine at Stanford Medicine. “Every public health department aligns with CDC policy—and on kids and Covid, the CDC is going to defer to the AAP.”
Convened in the early days of the coronavirus as a kind of emergency stopgap, the AAP’s Covid-19 response team had near dictatorial power over the organization’s pandemic policy. Typically, the AAP will not take a position without first soliciting feedback from all sections of the group that might be impacted by it—say, infectious diseases, endocrinology, and cardiology—to ensure the guidance reflects a thorough cost-benefit analysis.
That did not happen on the high-stakes issues posed by the pandemic. Instead, three knowledgeable AAP members said, the Covid-19 response team issued recommendations without consulting other parts of the AAP, in the hope of staying ahead of the virus.
“The norms for developing communications and policies are normally very robust,” a former AAP official said. “But the disaster framework subverted a lot of those norms.”
Multiple AAP higher-ups, including an officer in the cardiology section, which normally reviews all policies related to heart functioning, said their teams were never consulted about the group’s Covid recommendations, including the recommendations about the vaccine.
“At this point we knew about myocarditis,” the cardiologist said, “but they didn’t ask for our opinion.”
In an email to the Free Beacon and Common Sense, the AAP claimed to have consulted cardiologists “on a variety of topics” throughout the pandemic, but declined to specify whether the vaccine was one of them.
For some doctors, the response team’s composition was just as concerning as its lack of transparency. Several of its members, including Maldonado, work in children’s hospitals, which by definition see kids who are sicker than average, including from Covid.
The result, some AAP members said, is that the bureaucrats crafting Covid policy had a skewed perception of the disease’s pediatric risks, while rank-and-file pediatricians were seeing the 99.9 percent of kids who didn’t require hospitalization—at least not for the virus.
“Our psych unit was full the entire pandemic,” said Nicole Johnson, a doctor at University Hospitals Rainbow Babies & Children’s in Cleveland. “Kids were waiting for beds to open in the psych unit while there were no kids in the Covid ward.”
There was also a tendency, implicit in the response team’s mandate, to focus more on the effects of Covid than the consequences of lockdowns. Lockdowns, while not formally endorsed by the AAP, were not vigorously opposed by it either.
“Primary care physicians see kids gain weight as we try to keep them safe from Covid,” said Todd Porter, a pediatrician from Denver, Colorado who left the AAP over its Covid policies, adding that some of his patients put on more than 30 pounds during the pandemic. “But people in medical bureaucracies just see case counts.”
Opposing those bureaucracies—and the Covid policies they formulated—became a professional risk. One pediatrician said her bosses threatened to fire her for tweeting critically about the AAP’s vaccine recommendations. “They hauled me into the office and asked me if I wanted to work there,” the doctor said, adding that she knew of colleagues who were terrified of speaking out. Another pediatrician described how the president of her state AAP chapter told her to pipe down about Covid restrictions if she didn’t want to lose funding for an academic program.
“Had I replied ‘F you,’ I wouldn’t have gotten the grants, and I wouldn’t have been able to help my program,” the pediatrician said.
Trans Health Care: ‘The AAP says kids under 10 can’t cross the street by themselves, but they can change their gender’
The pandemic showed how a small group of like-minded doctors, acting with virtually no oversight, can push extreme policies through the AAP based on very little evidence. The group’s guidance on gender dysphoria offers a similar lesson.
In 2016, the AAP established a committee on “LGBT Health & Wellness” to support “children with variations in gender presentation.” Four of the committee’s six members—Jason Rafferty, Brittany Allen, Michelle Forcier, and Ilana Sherer—work in pediatric gender clinics that prescribe puberty blockers to patients as young as 10 and cross-sex hormones to patients as young as 14.
Those treatments are part of the broader model of “gender-affirming” care that the AAP endorsed in its 2018 policy statement, “Ensuring Comprehensive Care and Support for Transgender and Gender-Diverse Children and Adolescents.” The statement, which represents the official position of the AAP, was written by a single doctor, Rafferty, and does not appear to have been reviewed by anyone else at the organization: Rafferty “conceptualized,” “drafted,” “reviewed,” “revised,” and “approved” the manuscript himself, a note at the end of the paper reads. Rafferty did not respond to a request for comment.
“There was clearly no fact-checking,” one longtime AAP member said. “The AAP thought trans was the next civil rights crusade and got boondoggled by enthusiastic young doctors.”
The 2018 statement was an extraordinary departure from the international medical consensus. Most European countries do not encourage social or physical transition until a child’s gender dysphoria has persisted for quite some time—an approach known as “watchful waiting”—in part because the dysphoria desists on its own in the majority of cases, particularly once puberty hits.
Rafferty, however, called watchful waiting “outdated” and endorsed a “gender-affirming” paradigm, in which transitioning is on the table almost as soon as a child identifies as transgender. Some of the studies he cited to support that conclusion—including a practice guideline from the American Academy of Child and Adolescent Psychiatry—actually undercut it, arguing that, more often than not, “sex-reassignment” should be deferred until adulthood.
Though the policy statement conceded that puberty blockers may pose “long-term risks” to “bone metabolism and fertility,” it did not recommend any prerequisites for obtaining drugs. They could be given out at the earliest stages of puberty—meaning to children as young as nine—and, Rafferty insisted, were “reversible.”
Since then, the gap between the AAP and the rest of the world has only grown. Many European countries, including Britain, Finland, Sweden, and the Netherlands, are now curtailing or entirely eliminating the use of puberty blockers in children with gender dysphoria, citing both long-term health risks and a lack of evidence that they alleviate the condition. The AAP has nonetheless maintained its support for the drugs—which it claims have the backing of the “most prominent medical organizations worldwide”—while rejecting calls for more gatekeeping.
“The AAP says kids under 10 can’t cross the street by themselves,” one pediatrician said, referencing the group’s official recommendations on pedestrian safety, “but they can change their gender. How does that make sense?”
The contrast points to a broader tension within AAP guidance: On most kitchen table issues, from diet to screen time to exercise, the group has long encouraged a kind of safetyism, stressing the need for parental supervision and the pitfalls of pubescent judgment. Yet on trans issues, it has done nearly the opposite, suggesting that minors are mature enough to transition without their parents’ knowledge or consent.
“A family may deny access to care that raises concerns about the youth’s welfare and safety,” Rafferty’s statement says. “In such rare situations, pediatric providers may want to familiarize themselves with relevant local consent laws and maintain their primary responsibility for the welfare of the child.” It’s a stark departure from the way the group talks about other forms of body modification: one AAP report recommends that “adolescents speak with their parents” before getting tattoos, because they are “permanent,” “difficult to remove,” and “involve significant consequences.”
By 2019, Rafferty’s guidance was eliciting quiet concern among rank-and-file doctors affiliated with the AAP. “Normie pediatricians were like, ‘what’s going on,’” one doctor said, recalling the hushed conversations she had in the hallways of the AAP’s 2019 national conference, which featured a panel on gender-affirming care. Gender specialists, on the other hand, “considered themselves life-saving heroes.”
Rather than promoting dialogue or compromise between the two camps, the AAP sought to stifle dissent. In October, it urged the Department of Justice to investigate critics of “gender affirming” care, arguing they were spreading “disinformation” that puts lives at risk. That move came after the organization barred the Society for Evidence-based Gender Medicine, which advocates the watchful waiting approach, from being an exhibitor at its national conference last year. In August, it also blocked a resolution calling for a review of the AAP’s current guidance on puberty blockers, which the head of Boston Children’s Hospital’s gender clinic, Jeremi Carswell, says are “given out like candy” at her clinic.
The stifling of dissent has created an illusory medical consensus that nonetheless exerts extraordinary influence over public policy and debate. Courts have cited the AAP in cases about transgender children—Eknes-Tucker v. Marshall, for example, in which an Alabama District Court blocked a law banning puberty blockers, cross sex hormones, and gender reassignment surgeries for trangender minors (the case is now on appeal). Talking heads, meanwhile, have invoked the AAP to shut down criticism of childhood gender transition.
In October, Jon Stewart berated Arkansas attorney general Leslie Rutledge after her state passed a law similar to Alabama’s, arguing that she was bucking the AAP’s “peer-reviewed” guidelines. Banning puberty blockers would be as backwards as banning chemotherapy, Stewart said. He did not mention that the Swedish National Board of Health and Welfare had, in February, recommended halting hormonal gender treatment for minors except in tightly limited circumstances.
The National Institutes of Health has funded one study on the long-term effects of puberty blockers, which is being conducted by four university-affiliated gender clinics—including the one at Boston Children’s, the place that acknowledged prescribing blockers “like candy.” The study, which began in 2015, has yet to report its findings, and the authors have not declared any conflicts of interests.
The Death of Expertise
At stake in all this, said Marty Makary, a surgeon and public policy researcher at Johns Hopkins Medicine, is not just lockdowns or puberty blockers but the credibility of the medical establishment itself.
“The AAP still puts out many important recommendations that parents should follow,” Makary said, citing the group’s support for the measles vaccine and its guidance on preventing sudden infant death syndrome. “If parents start to distrust the AAP because of its politicization, I worry we’ll see more pediatric deaths.”
There is some evidence, albeit anecdotal, to justify Makary’s fears. In particular, several pediatricians said that the AAP’s zealotry around the Covid vaccine had raised parental concerns about other, more well-established vaccinations. One reported seeing “a lot more hesitancy around routine immunizations,” including for measles, after schools in her area started requiring the Covid vaccine based on the AAP’s guidance. Another said she’d been inundated with requests for a second opinion by parents who “who don’t trust their own physicians on vaccines,” both Covid and non-Covid.
“I have to tell them the other vaccines are good,” the pediatrician added.
Other doctors described families–including families in deep blue areas–who have developed a reflexive distrust of anything the AAP says.
“I now hear parents mock the AAP over even non-political guidance like breastfeeding recommendations,” a pediatrician in Portland, Oregon said. “They’re just tuning everything out.”
For Vinay Prasad, a professor of epidemiology and biostatistics at the University of California, San Francisco, it’s hard to blame them.
“The reason to trust modern doctors over ancient healers is that more of what we tell you to do is justified by well-done studies,” Prasad said. “But how do we hold that perch when we just make stuff up?”
Leave a comment