curated by Marilyn M. Singleton, M.D., J.D. – http://marilynsingletonmdjd.com/
Updated September 26, 2020 – for The Association of American Physicians and Surgeons

My cmnt: The upshot of this lengthy and well-documented article is that the wearing of masks by the general public does NOT stop the spread of any airborne virus (i.e., covid-19, colds or the flu), Covid-19 and the flu are also spread by touching contaminated surfaces (i.e., everything), that masks worn by the general public are not and cannot be fitted properly nor are they effective shields to the wearer or those around him, viruses enter thru the eyes so you would also have to wear an effective goggle (also not possible for the general public), masks are for show, masks have a number of negative consequences which are generally greater than the alleged benefits, if a mask is touched (and they always are) while putting it on or while wearing it is contaminated, if a mask has ANY air leakage (and they all do) it is useless, children (especially young children) should not ever wear masks for any extended length of time, and masks give a false sense of security which simply is not there. Read the entire article by clicking the above link.
Introduction
COVID-19 is as politically-charged as it is infectious. Early in the COVID-19 pandemic, the WHO, the CDC and NIH’s Dr. Anthony Fauci discouraged wearing masks as not useful for non-health care workers. Now they recommend wearing cloth face coverings in public settings where other social distancing measures are hard to do (e.g., grocery stores and pharmacies). The recommendation was published without a single scientific paper or other information provided to support that cloth masks actually provide any respiratory protection. Let’s look at the data.
The theory behind mask wearing:
- Source control: Cloth mask can trap droplets that come out of a person’s mouth when they cough or sneeze.
- Protection: Personal Protective Equipment (PPE) – only N95 masks
Transmission of SARS-CoV-2
Note: A COVID-19 (SARS-CoV-2) particle is 0.125 micrometers/microns (μm); influenza virus size is 0.08 – 0.12 μm; a human hair is about 150 μm.
*1 nm = 0.001 micron; 1000 nm = 1 micron; Micrometer (μm) is the preferred name for micron
*1 meter is = 1,000,000,000 [trillion] nm or 1,000,000 [million] microns
*For a complete dissection and explanation of aerosols and airborne particles, please see Understanding Particle Size and Aerosol-based Transmission by Steve Probst. https://www.4cconference.com/wp-content/uploads/2020/07/Understanding-Particle-Size-and-Aerosol-Based-Transmission.pdf
Droplets
- Virus is transmitted through respiratory droplets produced when an infected person coughs, sneezes, or talks.
- Larger respiratory droplets (>5 μm) remain in the air for only a short time and travel only short distances, generally <1 meter. They fall to the ground quickly.https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30245-9/fulltext
- This idea guides the CDC’s advice to maintain at least a 6-foot distance.
- Small (<5 μm) aerosolized droplets can remain in the air for at least 3 hours and travel long distances (up to 27 ft.).
Air currents
- In an air conditioned environment these large droplets may travel farther.
- Ventilation. Even the opening of an entrance door and a small window can dilute the number of small droplets to one half after 30 seconds. (This study looked at droplets from uninfected persons). This is clinically relevant because poorly ventilated and populated spaces, like public transport and nursing homes, have high SARS-CoV-2 disease transmission despite physical distancing.
Humidity
- Since 1961, experiments showed that viral-pathogen-carrying droplets were inactivated within shorter and shorter times as ambient humidity was increased. Dryness drives the small aerosol particles. See e.g., review of studies, https://aaqr.org/articles/aaqr-20-06-covid-0302
Conclusions
The preponderance of scientific evidence supports that aerosols play a critical role in the transmission of SARS-CoV-2. Years of dose response studies indicate that if anything gets through, you will become infected.
- Thus, any respiratory protection respirator or mask must provide a high level of filtration and fit to be highly effective in preventing the transmission of SARS-CoV-2. (Works for Mycobacterium tuberculosis (3μm)
- Public health authorities define a significant exposure to COVID-19 as face-to-face contact within 6 feet with a patient with symptomatic COVID-19 that is sustained for at least a few minutes (and some say more than 10 minutes or even 30 minutes).
- The chance of catching COVID-19 from a passing interaction in a public space is therefore minimal.
MASKS
Filter Efficiency and Fit
Data from a University of Illinois at Chicago review https://www.cidrap.umn.edu/news-perspective/2020/04/commentary-masks-all-covid-19-not-based-sound-data
- HEPA (high efficiency particulate air) filters are 99.97 to 100% efficient. HEPA filters are tested with particles that are 0.125 μm (the size of SARS-CoV-2).
- Masks and respirators work by collecting particles through several physical mechanisms, including diffusion (small particles) and interception and impaction (large particles).
- Surgical masks are loose-fitting devices that were designed to be worn by medical personnel to protect accidental contamination of patient wounds, and to protect the wearer against splashes or sprays of bodily fluids. They aren’t effective at blocking particles smaller than 100 μm. https://multimedia.3m.com/mws/media/957730O/respirators-and-surgical-masks-contrast-technical-bulletin.pdf
- OSHA/CDC: A surgical mask is not a respirator. It cannot be used to protect workers who perform or assist with aerosol-generating procedures, which may create very fine aerosol sprays. A surgical mask can only be used to protect workers from contact with the large droplets made by patients when they cough, sneeze, talk or breathe. https://www.osha.gov/dts/guidance/flu/healthcare.html
Laboratory Studies
- N95 filtering facepiece respirators (FFRs) are constructed from electret (a dielectric material that has a quasi-permanent electric charge.) An electret generates internal and external electric fields so the filter material has electrostatic attraction for additional collection of all particle sizes. As flow increases, particles will be collected less efficiently.
- A properly fitted N95 will block 95% of tiny air particles down to
0.3 μm from reaching the wearer’s face.- https://www.honeywell.com/en-us/newsroom/news/2020/03/n95-masks-explained.
- Problem: no source control. An N95 does not filter exhaled air passing through the exhaust/exhalation valve (for easier breathing and less moisture inside the mask).
- Study measuring filter efficiency (2010)
- https://academic.oup.com/annweh/article/54/7/789/202744; https://www.cidrap.umn.edu/news-perspective/2020/04/commentary-masks-all-covid-19-not-based-sound-data; https://academic.oup.com/annweh/article/54/7/789/202744
- Filter efficiency was measured across a wide range of small particle sizes (0.02 to 1 µm) at 33 and 99 L/min.
- All the cloth masks and materials had near zero efficiency at 0.3 µm, a particle size that easily penetrates into the lung (SARS-CoV-2 is 0.125 µm)
- Efficiency for the entire range of particles
- T-shirts — 10%
- Scarves — 10% to 20%
- Cloth masks — 10% to 30%
- Sweatshirts — 20% to 40%
- Towels — 40%
- Study measuring filter efficiency (2014, Korea)
- https://aaqr.org/articles/aaqr-13-06-oa-0201
- Evaluated 44 masks, respirators, and other materials with similar methods and small aerosols (0.08 and 0.22 µm)
- N95 FFR filter — >95% efficiency
- Medical masks — 55% efficiency
- General (cloth) masks — 38% efficiency
- Handkerchiefs — 2% (one layer) to 13% (four layers) efficiency.
- Conclusion: Wearing masks (other than N95) will not be effective at preventing SARS-CoV-2 transmission, whether worn as source control or as PPE.
- N95s protect health care workers, but are not recommended for source control transmission.
- Surgical masks are better than cloth but not very efficient at preventing emissions from infected patients. Cloth masks must be 3 layers, plus adding static electricity by rubbing with rubber glove.
- The cloth that serves as the filtration for the mask is meant to trap particles being breathed in and out. But it also serves as a barrier to air movement because it forces the air to take the path of least resistance, resulting in the aerosols going in and out at the sides of the mask.
- An August 2020 UCSF study suggested that the mask would decrease the absolute volume of the inoculum. (The concentrations of bacteria upstream and downstream of the test devices were measured with an aerodynamic size spectrometer) https://ucsf.app.box.com/s/blvolkp5z0mydzd82rjks4wyleagt036
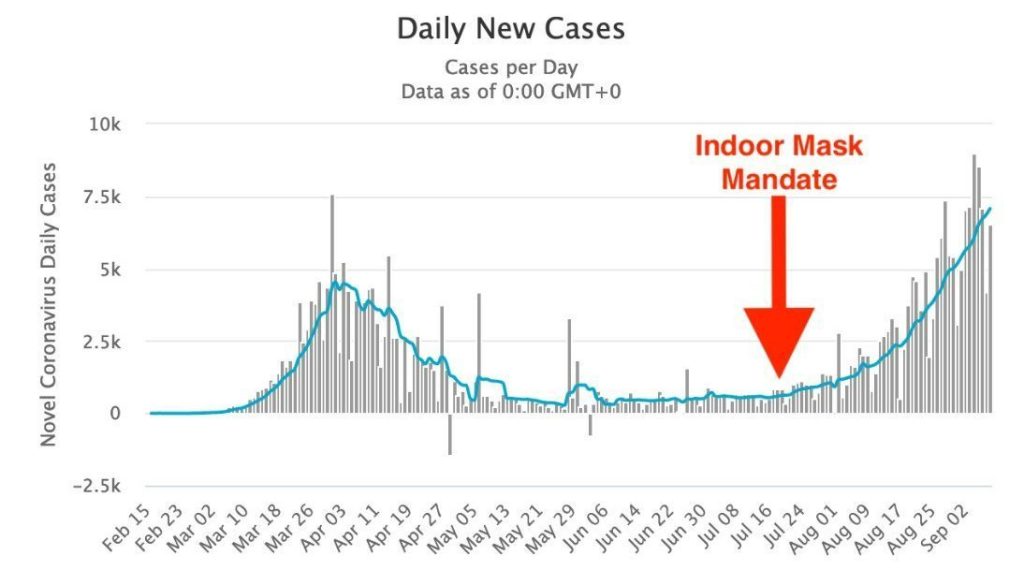
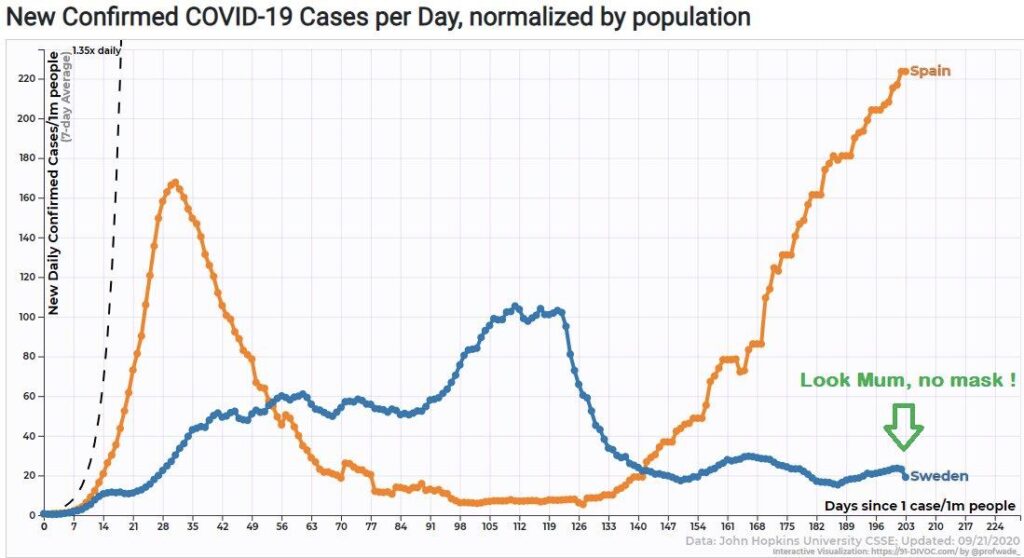
Negative Effects of Masks
Air inside the mask is definitely stale. In filtering particles, the mask makes it harder to breathe.
Decreased PaO2
- A 2004 observational study of end stage renal disease patients during dialysis for 4 hours (2004, Taiwan).
- https://pubmed.ncbi.nlm.nih.gov/15340662/;
- https://www.researchgate.net/publication/8371248_The_physiological_impact_of_wearing_an_N95_mask_during_hemodialysis_as_a_precaution_against_SARS_in_patients_with_end-stage_renal_disease
- 39 patients, mean age, 57 years. 70% had decreased PaO2 (from 100 to 92); 19% had hypoxemia (PaO2 <70); all patients had increased respiratory rate 16 to 18; chest discomfort (3 baseline patients to 11 patients); respiratory distress (1 baseline patient to 17 patients)
- Stanford engineers estimated that N95 masks cause a 5% to 20% reduction in O2 intake. This can cause dizziness and lightheadedness. This can be life-threatening for someone with lung disease or with respiratory distress.
- Study of surgeons in the OR (2008, Turkey).
- http://scielo.isciii.es/pdf/neuro/v19n2/3.pdf
- Scientists looked at O2 levels of surgeons wearing masks while performing surgery. Found a decrease in the oxygen saturation of arterial pulsations (peripheral capillary O2 saturation/SpO2) fell from 98% to 96% and a slight increase in pulse rates compared to preoperative values in all surgeon groups.
Increased CO2
- This may be merely theoretical. Carbon dioxide molecules freely diffuse through the masks, allowing normal gas exchange while breathing.
- CO2 is present in the atmosphere at a level of about 0.04% (400ppm). According to the U.S. Department of Agriculture / OSHA, carbon dioxide becomes toxic at concentrations above 4 percent (40,000ppm); symptoms at 5,000-10,000 ppm. 10,000 ppm has been measured behind mask.
- Experiment (July 2020).
- https://www.wthr.com/article/news/health/coronavirus/verify-do-face-masks-reduce-oxygen-intake-carbon-dioxide-experiment-multiple-maskss/531-c00c96cb-9273-4947-949c-0807f94454a7
- Pulse oximeter and exhaled CO2 (via tube in mask) No change with mask. (End-tidal capnography or end-tidal CO2 (EtCO2) monitoring is a non-invasive technique that measures the partial pressure or maximal concentration of carbon dioxide (CO2) at the end of an exhaled breath. The normal values are 5-6% CO2, which is equivalent to 35-45 mmHg.)
- Health care worker study (2005, Scandinavia)
- https://pubmed.ncbi.nlm.nih.gov/16441251/
- 37.3% reported face-mask-associated headaches, 32.9% reported headache frequency >6 times per month. 7.6% had taken sick leave from March 2003 to June 2004 (mean 2 days; range 1-4 days) and 59.5% required use of abortive analgesics because of headache.
- Health care worker study (2009, Japan) with similar headache results as Scandinavian study (above).
- While there are some articles reporting OSHA tests, it is not clear they were proper tests.
- Some people have mistakenly claimed that OSHA standards (e.g., the Respiratory Protection standard, 29 CFR 1910.134; the Permit-Required Confined Space standard 29 CFR 1910.146; and the Air Contaminants standard, 29 CFR 1910.1000) apply to the issue of oxygen or carbon dioxide levels resulting from the use of medical masks or cloth face coverings in work settings with normal ambient air (e.g. healthcare settings, offices, retail settings, construction). These standards do not apply to the wearing of medical masks or cloth face coverings in work settings with normal ambient air). These standards would only apply to work settings where there are known or suspected sources of chemicals (e.g., manufacturing facilities) or workers are required to enter a potentially dangerous location (e.g., a large tank or vessel). https://www.osha.gov/SLTC/covid-19/covid-19-faq.html
- It is hard to tell if the headaches experienced by HCWs with N95s is CO2 or having a strap around the head.
- But when asked should we be worried about CO2, mask proponents say, “No” because you can exhale around the sides of the mask. This defeats the purpose. (2006) https://pubmed.ncbi.nlm.nih.gov/16441251/
Moisture retention
- Reuse of cloth masks, frequency and effectiveness of cleaning, and poor filtration may result in increased risk of infection.
- Observations during SARS suggested double-masking and other practices increased the risk of infection because of moisture, liquid diffusion.
- Recent study (in German) cultured 82 bacterial colonies & 4 mold (fungoid) colonies from a child’s masks after 8 hours of wear.
Self-contamination
- Contamination through repeated use and improper doffing is possible. The virus may survive on the surface of the mask. The pathogen goes from mask to bare hands.
“Mask mouth”
- Reported by dentists. https://nypost.com/2020/08/05/mask-mouth-is-a-seriously-stinky-side-effect-of-wearing-masks/
- Wearing masks increases dryness, which leads to decrease in saliva. It is the saliva that fights bacteria. Result is decaying teeth, receding gum lines and seriously sour breath. Gum disease — or periodontal disease — will eventually lead to strokes and an increased risk of heart attacks.”
World Health Organization (WHO), June 2020
- https://apps.who.int/iris/bitstream/handle/10665/332293/WHO-2019-nCov-IPC_Masks-2020.4-eng.pdf?sequence=1&isAllowed=y
- “The likely disadvantages of the use of mask by healthy people in the general public include:
- potential increased risk of self-contamination due to the manipulation of a face mask and subsequently touching eyes with contaminated hands;
- potential self-contamination that can occur if non- medical masks are not changed when wet or soiled. This can create favourable conditions for microorganism to amplify;
- potential headache and/or breathing difficulties, depending on type of mask used;
- potential development of facial skin lesions, irritant dermatitis or worsening acne, when used frequently for long hours;
- difficulty with communicating clearly;
- potential discomfort;
- a false sense of security, leading to potentially lower adherence to other critical preventive measures such as physical distancing and hand hygiene;
- poor compliance with mask wearing, in particular by young children;
- waste management issues; improper mask disposal leading to increased litter in public places, risk of contamination to street cleaners and environment hazard;
- difficulty communicating for deaf persons who rely on lip reading;
- disadvantages for or difficulty wearing them, especially for children, developmentally challenged persons, those with mental illness, elderly persons with cognitive impairment, those with asthma or chronic respiratory or breathing problems, those who have had facial trauma or recent oral maxillofacial surgery, and those living in hot and humid environments.
The Hamburg Environmental Institute (July 2020) warned of the inhalation of chlorine compounds in polyester masks as well as problems in connection with face mask disposal. https://swprs.org/face-masks-evidence/; https://corona-transition.org/maskentragen-noch-ungesunder-als-gedacht (in German)
Psychological Damage in Children (September 11, 2020).
https://www.world-today-news.com/70-doctors-in-open-letter-to-ben-weyts-abolish-mandatory-mouth-mask-at-school-belgium/
- 70 Belgian doctors begged for cancellation of mask mandate at school. “In recent months, the general well-being of children and young people has come under severe pressure. We see in our practices an increasing number of children and young people with complaints due to the rules of conduct that have been imposed on them. We diagnose anxiety and sleep problems, behavioral disorders and fear of contamination. We are seeing an increase in domestic violence, isolation and deprivation. Many lack physical and emotional contact; attachment problems and addiction are obvious. ‘The mandatory mouth mask in schools is a major threat to their development. It ignores the essential needs of the growing child. The well-being of children and young people is highly dependent on the emotional connection with others. (…) The aim of education is to create an optimal context so that a maximum development of young people is possible. The school environment must be a safe practice field. The mouth mask obligation, on the other hand, makes the school a threatening and unsafe environment, where emotional connection becomes difficult. ‘In addition, there is no large-scale evidence that wearing face masks in a non-professional environment has any positive effect on the spread of viruses, let alone on general health.’
Unanswered questions
- Can virions escape an evaporating droplet stuck to a mask fiber?
- What are long-term health effects on HCW, such as headaches, arising from impeded breathing?
- Are there negative social consequences to a masked society?
- Are there negative psychological consequences to wearing a mask, as a fear-based behavioral modification?
- What are the environmental consequences of mask manufacturing and disposal?
Leave a comment